The Society for Academic Emergency Medicine (SAEM) Foundation awarded a $10,000 grant to Gannon University, which will help fund a project aimed at improving the survival rate of patients in cardiac arrest.
The proposal, titled “Comparison of Visual Centers of Attention between Experienced and Novice Providers during a Simulated Cardiac Arrest,” will study how teams of medical professionals work together during cardiac arrest resuscitation.
Jestin Carlson, M.D., the principal investigator for the project and adjunct lecturer at Gannon as well as the resident research director at Saint Vincent Hospital, and his co-principal investigator, Adam Frisch, M.D., M.S., assistant professor of emergency medicine in the Department of Emergency Medicine at Albany Medical College, will study how novice and more experienced care providers see and react to situations that arise during a resuscitation.
Shanen Lazenby, a junior respiratory therapy major, said she is very optimistic about the grant and its uses in the patient simulation center.
“This study will greatly benefit Gannon’s health care education because instructors will be able to better identify weak spots in resuscitations,” Lazenby said.
Carlson said if someone is experienced, they can incorporate what they’ve seen and act on it.
“If you’re not experienced, you don’t know what to focus on, so we ultimately want to teach novice providers how to develop those skills to make them more effective in a clinical setting,” Carlson said.
Emily Nottingham, a junior respiratory therapy major, said she cannot wait for the project to begin and put into use.
“This project is a great idea for both the students and the instructors,” Nottingham said. “This learning process, when being a student or an instructor, is a great way to challenge the curriculum of the health care professions and, in turn, create a better health care education for Gannon.”
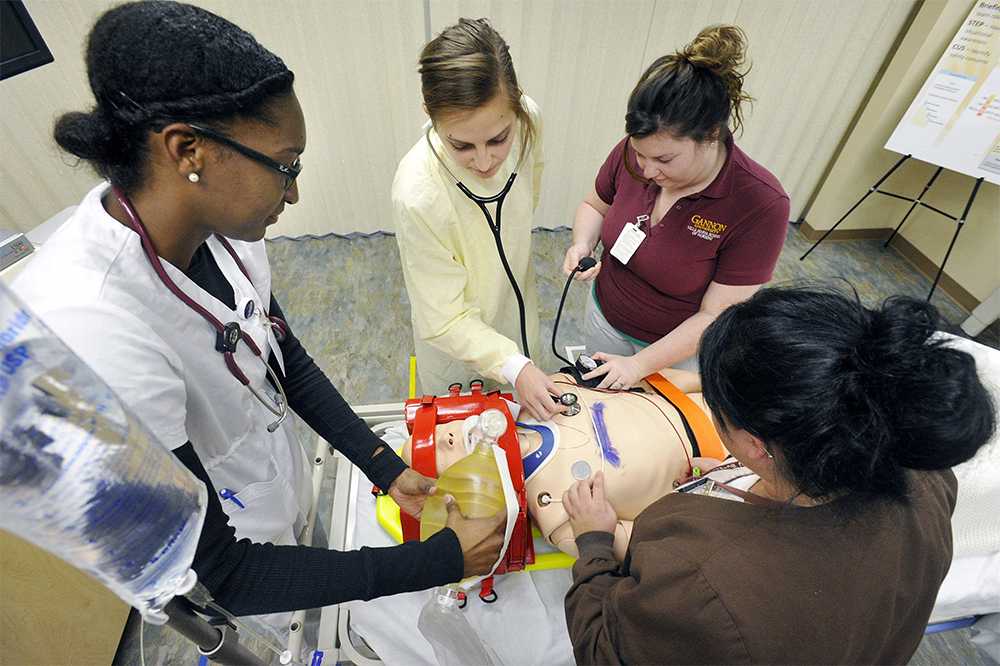
The center allows students from various health science disciplines to work together, as they would in a real-world clinical setting-precisely the kind of environment Carlson needs for his study.
Carlson said that a multidisciplinary team of providers is necessary to effectively resuscitate a patient – one putting in the IV, another administering medications and yet another ready to perform CPR.
“I’d like to impact the education process for health care providers – not just nurses and doctors, but the [entire] team,” Carlson said.
“The overall survival rate for patients who suffer a cardiac arrest outside a clinical setting is about 7 percent, but even small benefits can impact a large number of people.”
Carlson will work with Valerie Baker, a Gannon nursing professor, and together they will simulate cardiac arrests using the simulation center’s lifelike manikins and record the reactions of provider teams for later analysis.
Carlson said that the long-term goal of this project is to educate providers and save the lives of patients.
Lazenby said in a professional setting, the resuscitation team must work together to save the patient and having the stimulator will generate that experience.
“With the implementation of this grant to the patient simulation center, a wide variety of health care professions can collaborate and practice working as a team under analysis before they are in their fields working on real patients,” she said.
ANITA PEDUTO